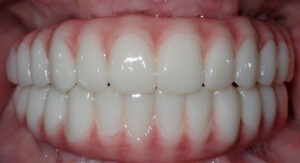
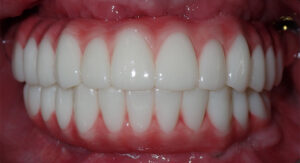
Proper dental implant aftercare involves a series of steps patients follow post-surgery to encourage healing, support osseointegration, and ensure your implants last for years. This diligent care helps prevent issues like peri-implantitis, loose restorations, and delayed bone fusion by managing infection, mechanical stress, and lifestyle factors that can hinder recovery. Written with a clinical perspective, this guide covers immediate post-operative actions, the biological healing timeline, daily cleaning practices, common complications and how to spot them, and strategies for long-term maintenance. You’ll discover clear, actionable advice for the first 24–72 hours, week-by-week expectations for soft tissue and bone healing, precise cleaning techniques using implant-safe tools, and what symptoms warrant immediate dental attention. The article also outlines professional maintenance schedules and lifestyle adjustments that enhance outcomes, and it highlights how specialized implant types influence aftercare. Throughout, keywords like dental implant aftercare, osseointegration timeline, swelling after implant surgery, dental implant hygiene routine, and peri-implantitis symptoms are woven in to provide you with practical, clinician-approved guidance.
What Are the Immediate Post-Operative Care Steps After Dental Implant Surgery?
Immediate post-operative care following dental implant surgery includes managing bleeding, resting, using cold therapy, controlling pain, and making early modifications to your oral hygiene routine to protect the initial blood clot and reduce inflammation. These actions work by minimizing tissue trauma, limiting bacterial exposure, and stabilizing the surgical site so soft tissue can close and osseointegration can begin. The practical outcome is reduced discomfort, a lower risk of infection, and an optimal environment for bone to fuse with the implant. Carefully follow these initial steps to establish a strong foundation for predictable healing and to minimize the chance of early complications.
How Should You Manage Pain and Swelling After Implant Placement?
Pain and swelling after implant surgery are normal inflammatory responses to tissue injury and can be effectively managed with a comprehensive approach combining medication, cold therapy, and proper positioning. For most patients, over-the-counter pain relievers like acetaminophen or ibuprofen can alleviate discomfort; any prescribed pain medication should be used exactly as directed and discussed with your clinician to prevent interactions. Apply a cold compress to the outside of your cheek for 20-minute intervals during the first 24–48 hours to help reduce swelling, then switch to warm compresses after 48–72 hours if stiffness persists. Keep an eye out for increasing pain, spreading swelling, fever, or drainage—these signs may indicate an infection or another complication and require prompt evaluation.
What Foods and Drinks Are Recommended Right After Surgery?
Opt for soft, nutrient-rich foods that require minimal chewing to protect the surgical site and support healing by providing essential calories and protein without placing mechanical stress on the implant area. Recommended choices include plain yogurt, smoothies (without straws), mashed potatoes, eggs, blended soups (cooled to a safe temperature), and soft-cooked cereals. Avoid hot liquids, spicy foods, and anything crunchy or sticky, as these can dislodge blood clots. Stay well-hydrated with still water and refrain from alcohol and tobacco during the early healing period, as these substances can impair tissue perfusion and immune response. Gradually reintroduce firmer foods as you feel comfortable, following your clinician’s guidance and observing visible healing progress.
- Recommended soft foods and drinks for immediate recovery:
- Plain yogurt and cottage cheese for protein and ease of consumption.
- Smoothies prepared without straws to prevent suction on the implant site.
- Mashed potatoes and well-cooked vegetables for calories and fiber.
These soft-food selections ensure you maintain good nutrition while minimizing mechanical stress. Transition back to a broader diet as your clinician confirms your healing progress.
How Do You Maintain Oral Hygiene in the First 24-48 Hours?
Early oral hygiene efforts focus on protecting the blood clot and preventing infection while keeping surrounding teeth and soft tissues clean through gentle methods that avoid direct trauma to the surgical site. For the first 24–48 hours, avoid vigorous brushing of the surgical area. Instead, gently clean non-operated teeth and use a prescribed antimicrobial rinse or a warm salt-water rinse after 24 hours to reduce bacterial levels. When you resume brushing near the implant, use a soft-bristled toothbrush with light, circular motions to avoid disturbing sutures or the healing gumline. Report any persistent bleeding, unpleasant taste, or increasing discharge so your dental team can assess if further intervention is needed.
How Long Does Dental Implant Healing Take and What Is the Osseointegration Process?
Dental implant healing involves both soft tissue closure and a longer osseointegration phase, during which bone remodels and fuses directly with the implant surface, providing mechanical stability and the ability to bear functional loads. Osseointegration is a biological fusion process where bone-forming cells deposit bone onto the implant fixture, creating direct bone-to-implant contact that stabilizes the restoration. The expected outcome is a durable foundation for crowns, bridges, or full-mouth restorations that can function like natural teeth once integration is complete. Understanding the timeline helps patients set realistic expectations for activity levels, diet, and the follow-up appointments needed to confirm successful integration.
Healing Phase | Key Process | Typical Timeline |
Soft tissue healing | Closure of the gums and reduction of swelling | 1–2 weeks |
Early bone remodeling | Initial bone formation around the implant surface | 4–12 weeks |
Osseointegration | Bone maturation and direct bone-to-implant contact | 3–6 months |
Prosthetic loading | Final crown/bridge attachment after sufficient stability is achieved | Timing based on clinical integration assessment |
What Are the Stages of Dental Implant Healing Week-by-Week?
Week-by-week healing begins with immediate clot formation and soft tissue sealing, progresses through a gradual reduction in swelling and tissue maturation, and continues into bone remodeling that steadily increases implant stability. Days 1–7 focus on controlling bleeding, managing swelling, and gentle oral hygiene. Weeks 2–6 typically involve suture removal (if applicable), reduced tenderness, and early bone deposition. Months 2–6 are characterized by bone maturation and increasing mechanical stability, leading up to when clinicians can safely place definitive restorations. The speed of recovery varies depending on overall health, bone quality, surgical complexity, and patient behaviors like smoking or poor blood sugar control. Keeping detailed notes of your symptoms and scheduled follow-ups helps clinicians monitor this progression and adjust timelines for placing restorations as needed.
How Does Osseointegration Affect Implant Stability?
Osseointegration is the primary determinant of long-term implant stability, transforming the implant from a foreign object into a biomechanically integrated part of the jawbone, allowing chewing forces to transfer into the bone without micro-movement. Successful integration minimizes the risk of implant mobility and prosthetic failure because bone remodeling creates a rigid interface around the implant’s surface. Clinical indicators of good osseointegration include the absence of mobility, decreasing discomfort, and stable bone levels visible on X-rays. Clinicians assess stability through clinical tests and imaging—information that guides the transition from healing abutments to final restorations. Understanding these assessments clarifies why staged follow-up appointments are crucial for the safe placement of restorations.
Following discussions on osseointegration timing and monitoring, please note that Dr. Igor Kaplansky provides personalized follow-up schedules for patients, assessing bone integration through clinical checks and imaging. Patients treated at our practice can expect tailored timelines based on their bone quality and implant type, whether standard fixtures or specialized options like zirconia or zygomatic implants, ensuring prosthetic work proceeds only after confirmed stability.
When Can You Resume Normal Activities and Diet?
Resuming normal activities and diet follows a phased approach aligned with soft tissue healing and osseointegration milestones to prevent excessive mechanical load or infection risk. Light activities and non-contact exercises can typically resume after 48–72 hours for uncomplicated cases, while strenuous activities or contact sports should be postponed until your clinician confirms adequate healing—often several weeks. Your diet can advance from liquids and soft foods to normal consistencies as swelling subsides and any sutures are managed. Definitive heavy chewing should wait until the implant has sufficient bone support. If you experience symptoms like increased pain or mobility as you reintroduce activities, revert to more conservative behaviors and contact your dental team.
What Is the Best Daily Cleaning Routine to Maintain Dental Implants?
The optimal daily cleaning routine for dental implants involves brushing twice a day, cleaning between your teeth daily, and occasionally using a water flosser or antimicrobial rinse as recommended to remove biofilm and prevent peri-implant disease. These practices work by disrupting plaque formation around the implant fixture and abutment, preserving healthy gum tissue and preventing inflammatory bone loss. The intended benefit is long-term health of the tissues around your implant, fewer complications, and extended prosthesis lifespan. The following guidance details the techniques, tools, and frequency for a reliable implant-specific hygiene routine.
How Do You Properly Brush and Floss Around Dental Implants?
Proper brushing and flossing around implants requires a gentle technique to clean the prosthetic margins without aggressive scrubbing that could irritate soft tissues or damage restorative materials. Use a soft-bristled toothbrush with light, circular strokes, angling the bristles at the implant margin to dislodge plaque while avoiding harsh horizontal scrubbing. Electric toothbrushes with soft heads can help ensure consistent pressure. For cleaning between teeth, use implant-specific floss, floss threaders, or small interdental brushes designed for implants to effectively clean contact areas. Gently slide the cleaner and avoid twisting motions that could snag restorations. Regularly ask your clinician for demonstrations and technique adjustments to suit your specific restoration design.
Developing a patient-centered approach to peri-implant maintenance therapy is essential as dental implants become more prevalent, recognizing that implant disease is influenced not only by microbes but also by numerous clinical and patient-related factors.
Dental Implant Maintenance Protocols: Patient-Focused Peri-Implant Therapy
As increasing number of dental implants are being placed in the general population, the need to develop a maintenance protocol that caters to the needs of the patients has become essential. Historically, dental implants were predominantly placed in the early edentulous population; however, the shift of placements to the wider population means that a patient-focused approach to peri-implant maintenance therapy (PIMT) and the effect this has on biological complications and implant survival need to be considered. This has been considered in the new periodontal classification (2017), which includes peri-implant diseases and conditions for the first time. Lang et al. [7] discussed Cumulative Interceptive Therapy (CIST), which suggested that the prevention of implant disease was better than the management of the disease itself. However, it is crucial to acknowledge that implant disease does not arise purely from microbes and the body’s inflammatory response to them. As stated by Albrektsson and his colleagues, there are numerous additional factors that contribute to implant failure and disease, encompassing various clinical and patient-related factors. Clearly, it is imperative that we educate our implant patients on how to clean their implant superstructures and abutments; however, as clinicians, we need to be cognizant of the fact that the pellicle that develops on titanium, either the implant surface itself or the implant abutment, differs from that which develops on enamel and cementum. In 1996, Edgerton demonstrated that a high-weight proline-rich glycoprotein pellicle forms on the dental implants, and this may contribute to the difference in the adhesion rates of the pellicles and also the type of specific bacteria found in implant crevices and surfaces.
Implant Maintenance and Aftercare, 2024
Which Oral Hygiene Tools Are Recommended for Implant Care?
Selecting the appropriate hygiene tools for implants helps remove plaque while protecting soft tissues and prosthetic surfaces. Recommended tools include soft-bristled toothbrushes, implant-safe interdental brushes, water flossers, and antiseptic rinses when advised. Below is a concise comparison of common tools to help you choose the right devices for your daily care routine.
Tool | Best Use | Recommended Frequency |
Soft-bristled toothbrush | Mechanical plaque removal on crowns and gumline | Twice daily |
Interdental brush (implant-safe) | Cleaning between implant restorations and natural teeth | Daily |
Water flosser | Removing debris around abutments and hard-to-reach areas | Daily or as an adjunct |
Antimicrobial mouthwash | Short-term infection control when prescribed | As directed (not indefinitely) |
How Often Should You Use Antimicrobial Mouthwash or Salt Water Rinses?
Antimicrobial mouthwash and salt water rinses serve distinct purposes during healing and maintenance. Saline rinses promote gentle cleansing immediately after surgery, while prescription antiseptic rinses like chlorhexidine are reserved for short-term use under clinician guidance to manage bacterial levels. Salt-water rinses can be used multiple times daily during the first week to soothe tissues and reduce surface contamination without disrupting healing. Chlorhexidine, on the other hand, is typically prescribed for limited courses to address elevated infection risk and should not be used long-term due to potential staining and alteration of oral flora. For ongoing maintenance, rely primarily on mechanical cleaning and reserve antiseptic rinses for episodic therapy as advised by your dental professional.
What Are Common Dental Implant Complications and How Can You Recognize Them?
Common dental implant complications include peri-implantitis, surgical site infection, prosthetic screw loosening, implant mobility, and, less frequently, nerve or sinus-related issues. Recognizing early signs allows both patients and clinicians to intervene before irreversible bone loss occurs. These conditions manifest through symptoms such as persistent bleeding, pus, increasing pain, radiographic bone loss, or visible mobility, and they can progress by eroding supporting bone or destabilizing prosthetics if left unmanaged. The clinical benefit of early recognition is clear: prompt treatment can preserve the implant and surrounding structures. The table below summarizes typical complications, their symptoms, and recommended immediate responses to guide your actions.
Condition | Symptom | Recommended Immediate Response |
Peri-implantitis | Bleeding when probed, swelling, pus discharge | Contact your dental office for assessment and professional cleaning |
Infection | Increasing pain, fever, unpleasant taste | Seek urgent dental evaluation; antibiotics may be prescribed |
Loose implant or prosthesis | Mobility, shifting bite | Avoid chewing on that side and call for an emergency evaluation |
Nerve-related symptoms | Numbness or tingling beyond the expected recovery period | Contact your clinician promptly for assessment and imaging |
What Are the Signs and Symptoms of Peri-Implantitis and Infection?
Peri-implantitis typically begins with inflammation of the soft tissues around the implant and can progress to pus formation and radiographic bone loss if left untreated. Therefore, identifying and addressing early signs is critical. Patients might notice bleeding during brushing or probing, persistent localized swelling, a bad taste or discharge, increased pain beyond expected post-operative levels, or changes in how the restoration feels. Clinicians confirm progression through clinical probing and X-rays. Early-stage peri-implant mucositis is often reversible with improved hygiene and professional cleaning, while established peri-implantitis may require surgical intervention. Document your symptoms, take photos if helpful, and contact your dental team for prompt assessment.
Understanding the causes, diagnosis, and treatment of peri-implantitis is crucial, as it is an infectious condition that leads to inflammation and bone loss around a functional implant, with microorganisms like spirochetes and Gram-negative anaerobes often being implicated.
Understanding and Managing Peri-Implantitis: Causes, Diagnosis, and Treatment
Peri-implantitis is a site-specific infectious disease that causes an inflammatory process in soft tissues, and bone loss around an osseointegrated implant in function. The etiology of the implant infection is conditioned by the status of the tissue surrounding the implant, implant design, degree of roughness, external morphology, and excessive mechanical load. The microorganisms most commonly associated with implant failure are spirochetes and mobile forms of Gram-negative anaerobes, unless the origin is the result of simple mechanical overload. Diagnosis is based on changes of color in the gingiva, bleeding and probing depth of peri-implant pockets, suppuration, X-ray, and gradual loss of bone height around the tooth. Treatment will differ depending upon whether it is a case of peri-implant mucositis or peri-implantitis. The management of implant infection should be focused on the control of infection, the detoxification of the implant surface, and regeneration of the alveola
Management of peri-implantitis, 2012
How Should You Respond to Loose Implants or Persistent Pain?
A loose implant or persistent, worsening pain signals compromised stability or infection and requires prompt evaluation to prevent further damage and to preserve adjacent bone and tissues. If you detect mobility or a restoration that shifts, avoid chewing on that side, refrain from manipulating the area, and contact your dental provider immediately for imaging and potential stabilization or removal. Persistent pain that is not relieved by appropriate medications and is accompanied by swelling or fever raises concern for infection and typically warrants urgent clinical evaluation and treatment planning. Swift action reduces the likelihood of implant loss and accelerates recovery.
What Risk Factors Increase the Chance of Implant Failure?
Several modifiable and non-modifiable risk factors can increase the probability of implant failure by impairing healing, raising infection risk, or diminishing bone quality. Key contributors include smoking, uncontrolled diabetes, poor oral hygiene, untreated periodontal disease, and insufficient bone volume. Smoking reduces blood flow and compromises immune response, significantly increasing complications and reducing osseointegration success, while systemic conditions like uncontrolled diabetes affect wound healing and infection control. Certain medications (e.g., bisphosphonates) and bruxism (teeth grinding) can also alter the mechanical and biological environments around implants. Identifying and managing these risks before and after surgery supports better outcomes through behavioral changes, medical coordination, or alternative surgical planning.
How Can You Protect Your Dental Implants for Long-Term Success?
Long-term protection of your dental implants relies on consistent home care, scheduled professional maintenance, lifestyle adjustments, and tailored approaches for specific implant types to prevent peri-implant disease and mechanical complications. These strategies work by maintaining low levels of bacterial biofilm, controlling forces on restorations, and enabling early detection of tissue or prosthetic changes that signal potential problems. The resulting benefits include stable bone levels, preserved soft tissue contours, and functional restorations that last for many years. Next, we’ll detail why regular check-ups, specific lifestyle changes, and material-dependent aftercare are crucial for durability.
Why Are Regular Dental Check-Ups Crucial for Implant Longevity?
Regular dental check-ups allow professionals to remove hardened deposits, assess prosthetic fit, monitor radiographic bone levels, and detect early signs of soft tissue inflammation before they progress to peri-implantitis. Professional maintenance typically includes targeted cleaning with implant-safe instruments and evaluation of occlusion and prosthetic components to identify mechanical wear or screw loosening. The recommended frequency for these visits often ranges from every three to six months, depending on individual risk factors, plaque control, and periodontal history. These appointments are a proactive measure to sustain your oral health. For patients seeking structured maintenance, the practice led by Dr. Igor Kaplansky offers professional implant cleanings and personalized follow-up intervals as part of comprehensive dental implant services and full-mouth restoration planning.
Investigating the implant-related training and clinical practices of oral health professionals in Australia highlights the importance of understanding their role in providing peri-implant services and the protocols they follow for oral hygiene instructions and maintenance.
Australian Dental Implant Hygiene and Maintenance Practices Survey
Dental implant care and maintenance is of critical importance as implants grow in popularity as a tooth replacement option. The purpose of this study was to investigate the implant-related training and clinical practices of oral health practitioners (OHPs) in Australia regarding oral hygiene instructions (OHI) and maintenance protocols, and to better understand their role in providing peri-implant services.Methods:A 42-item web-based survey was forwarded to the members of the Dental Hygienists Association of Australia and the Australian Dental and Oral Health Therapists’ Association. Survey items included participant’s demographics, types of peri-implant services provided in the workplace, implant-related information sources, peri-implant diagnostic preferences, implant maintenance protocols and oral hygiene instructions (OHI) for dental implants. Descriptive statistics were used to analyse the data. Comparisons were made with a similar survey of the implant maintenance
Dental Implant Hygiene and Maintenance Protocols: A survey of oral health practitioners in Australia, MS Hopcraft, 2021
What Lifestyle Changes Support Healthy Implants?
Lifestyle adjustments that enhance implant outcomes include quitting smoking, optimizing blood sugar control for diabetic patients, making dietary choices that support tissue health, and addressing bruxism with night guards to minimize prosthetic overload. Smoking cessation improves tissue perfusion and immune function, which aids osseointegration and reduces infection risk. Similarly, managing systemic conditions helps prevent delayed healing. Controlling parafunctional habits like teeth grinding reduces mechanical wear and the risk of fracture for implant crowns and bridges. Combining these changes with consistent home care increases the predictability and longevity of implant-supported restorations.
How Do Zirconia and Zygomatic Implants Affect Aftercare Needs?
Zirconia implants and zygomatic implants are specific types of implant options that come with unique surgical and maintenance considerations, influencing aftercare protocols and the intensity of monitoring. Zirconia implants, favored for their aesthetic qualities, require meticulous soft-tissue hygiene to maintain color stability and peri-implant health. Zygomatic implants—used in cases of significant maxillary bone loss—necessitate more extensive and intensive monitoring due to complex anatomy and their proximity to sinus structures. Clinicians adapt maintenance protocols based on implant material and surgical approach, balancing prosthetic accessibility for cleaning with the protection of delicate peri-implant tissues. Understanding these distinctions helps patients adhere to appropriate long-term care plans.
What Are the Do’s and Don’ts of Dental Implant Aftercare?
A focused checklist of do’s and don’ts provides patients with practical, easy-to-remember guidelines to follow daily and during the initial healing period to prevent common complications and support osseointegration. These precautions work by limiting mechanical disruption, reducing bacterial exposure, and controlling systemic factors that can hinder recovery. Use the lists below as quick references for immediate and ongoing behaviors that protect your implant investment.
The essential daily aftercare do’s include:
- Brush twice daily with a soft-bristled brush, using gentle circular motions around the implant area.
- Clean between your teeth once daily using implant-safe interdental brushes or specialized floss techniques.
- Attend all scheduled professional maintenance visits for thorough cleaning and clinical monitoring.
Habits to avoid to prevent complications:
- Avoid smoking and alcohol during the healing phase, as they impair tissue blood flow and immune response.
- Avoid chewing on hard objects and using your teeth as tools, which can fracture restorations or transmit damaging forces to the implant.
- Avoid aggressive rinsing, forceful spitting, or using straws immediately after surgery, as these actions can dislodge blood clots.
When Should You Contact Your Dentist About Dental Implant Concerns?
Contact your dentist promptly if you experience red-flag symptoms such as severe or increasing pain not relieved by medication, spreading facial swelling, fever, persistent drainage, or any mobility of the implant or restoration. These signs often indicate infection, prosthetic failure, or other urgent issues requiring clinical evaluation. Early contact enables timely interventions, which may include imaging, antibiotics, professional cleaning, or prosthetic adjustments to prevent progression. When you call, provide a concise summary of your symptoms, recent changes, and any photos that illustrate swelling or prosthetic movement to help the clinician assess the urgency and plan the next steps efficiently.
What Symptoms Require Immediate Dental Attention?
Immediate dental attention is necessary for severe, worsening pain that is not managed by recommended analgesics, uncontrolled bleeding, visible pus or drainage, rapidly expanding swelling, fever, or any sudden mobility of an implant or prosthetic component. Before coming to the office, avoid touching or probing the area, control oral bleeding with gentle pressure if safe, and use prescribed medications as directed. Do not attempt to reposition loose restorations yourself. These emergency signs can indicate an infection that may spread or a failing implant that, if left untreated, could jeopardize adjacent structures. Timely clinical assessment minimizes complications and preserves treatment options.
How Does Dr. Kaplansky Support Patients During Aftercare?
Dr. Igor Kaplansky and the practice offer structured aftercare pathways that include scheduled follow-ups, availability for emergency triage, patient education resources, and personalized monitoring to track osseointegration and prosthetic function. The practice prioritizes patient education with demonstrations and materials illustrating optimal brushing, flossing, and maintenance techniques. We also coordinate care for complex cases, including zirconia implants, zygomatic implants, full-mouth restorations, and immediate solutions like TeethNow when clinically appropriate. If you experience concerning symptoms or require routine professional cleanings, our team is here to support you in scheduling evaluations and creating personalized aftercare plans that align with your clinical needs and lifestyle.
Frequently Asked Questions
What Should You Avoid After Dental Implant Surgery?
After dental implant surgery, it’s crucial to avoid certain activities to ensure proper healing. Refrain from smoking and consuming alcohol, as both can impair blood flow and immune response, increasing the risk of complications. Additionally, avoid hard, crunchy, or sticky foods that could dislodge the blood clot or put undue stress on the implant. It’s also important to steer clear of vigorous physical activities or heavy lifting for at least a few days post-surgery to prevent unnecessary strain on the surgical site.
How Can You Tell If Your Implant Is Failing?
Signs of a failing dental implant may include persistent pain, swelling, or discomfort around the implant site, as well as mobility of the implant or prosthetic. Other indicators include bleeding or pus around the implant, changes in bite alignment, and increased sensitivity. If you notice any of these symptoms, it’s essential to contact your dental provider immediately for evaluation. Early detection and intervention can help preserve the implant and surrounding bone structure, preventing further complications.
What Is the Role of Professional Cleanings in Implant Care?
Professional cleanings play a vital role in maintaining the health of dental implants. During these visits, dental professionals can remove plaque and tartar buildup that regular brushing may miss, assess the fit of the prosthetic, and monitor bone levels through radiographs. Regular cleanings help prevent peri-implant diseases and ensure that any potential issues are addressed early. Typically, patients should schedule these cleanings every three to six months, depending on individual risk factors and oral hygiene practices.
Can You Use Regular Toothpaste on Dental Implants?
While you can use regular toothpaste on dental implants, it’s advisable to choose a non-abrasive formula to avoid scratching the implant surface. Some patients prefer using toothpaste specifically designed for sensitive teeth or those with dental work, as these are often gentler. Additionally, using a soft-bristled toothbrush can help protect the implant and surrounding tissues. Always consult your dentist for recommendations tailored to your specific implant type and oral health needs.
How Does Diet Impact Dental Implant Success?
Your diet significantly impacts the success of dental implants. A balanced diet rich in vitamins and minerals supports healing and osseointegration. Foods high in calcium and vitamin D, such as dairy products, leafy greens, and fatty fish, are particularly beneficial for bone health. Conversely, avoid sugary and acidic foods that can promote bacterial growth and inflammation. Staying hydrated is also essential, as it aids in overall recovery. Discuss dietary recommendations with your dentist to optimize your implant success.
What Should You Do If You Experience Increased Sensitivity After Implant Placement?
Increased sensitivity after dental implant placement can be a normal part of the healing process, but it should be monitored closely. If sensitivity persists or worsens, contact your dentist for an evaluation. They may check for signs of infection, improper fit of the prosthetic, or other complications. In the meantime, using desensitizing toothpaste and avoiding extremely hot or cold foods can help manage discomfort. Always follow your dentist’s advice regarding sensitivity and any necessary adjustments.
How Can You Ensure Long-Term Success of Your Dental Implants?
To ensure the long-term success of your dental implants, maintain a rigorous oral hygiene routine that includes gentle brushing and interproximal cleaning. Regular dental check-ups are essential for professional cleanings and monitoring. Additionally, make lifestyle changes such as quitting smoking, managing diabetes, and eating a balanced diet to support healing and prevent complications. Staying informed about your implant care and promptly addressing any concerns with your dentist will also contribute to the longevity of your implants.